NeuroHope Presents at APTA National Conference
The NeuroHope story was presented at the American Physical Therapy Association’s (APTA) Combined Sections Meeting in Denver, Colorado on February 14th!
Preliminary findings of our ongoing research study were shared at the APTA’s annual summit where thousands of physical therapists and researchers from around the globe gather to share the latest developme
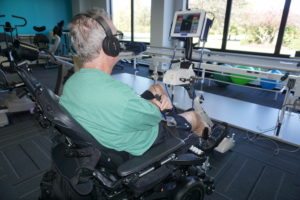
It was an exciting opportunity to showcase our unique mission and program. NeuroHope was created with a model that defies traditional healthcare. Instead of relying solely on insurance reimbursement and billable hours – we focus on patient access and affordability above everything else. Maximal recovery from catastrophic injuries depend on this standard of care, but adequate access to therapy, exercise, and expensive rehabilitative technology is difficult for healthcare systems to provide. The irony: knowledge, science, and rehabilitative technology is advancing, but patient access is declining.
Most people recovering from life-changing spinal cord and brain injuries stop therapy when insurance coverage is depleted, which may only be a few months following injury. The severity of neurologic injuries, the length of time needed to recover from them, and the lack of long-term quality of life programs in most communities leaves a void in care that NeuroHope was created to address.
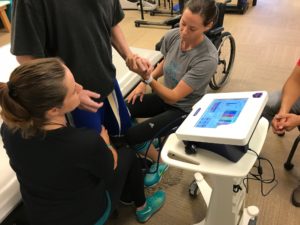
Thanks to support from the Indiana Spinal Cord and Brain Injury Research Fund, NeuroHope has partnered with a research team from the University of Indianapolis to track the long-term outcome measures of patients that have access to NeuroHope’s model of ongoing care. Since January 2018, patients attending NeuroHope have been evaluated extensively to monitor their motor fuction, physical activities and health-related quality of life during participation in our program. Patients with varying degrees of injuries, ages, and length of time since the injury, all participate in a rigorous 2-hour evaluation that consists of tests that measure neurologic function, balance, range of motion, reach, endurance, and walking, in addition to surveys to monitor their satisfaction and quality of life. Tests are repeated every 3 to 6 months to evaluate progress.
Patients are being tracked through the summer of 2020 in order to capture the clearest picture we can, but even now, preliminary results have shown improvements across most outcomes. In the coming months, we look forward to sharing complete results over a three-year period to gauge the effect that continued therapy and aggressive exercise may have for both recent and chronically injured patients recovering from neurologic injury.
Thanks to our supporters and partners, we are making affordable rehabilitation a reality!