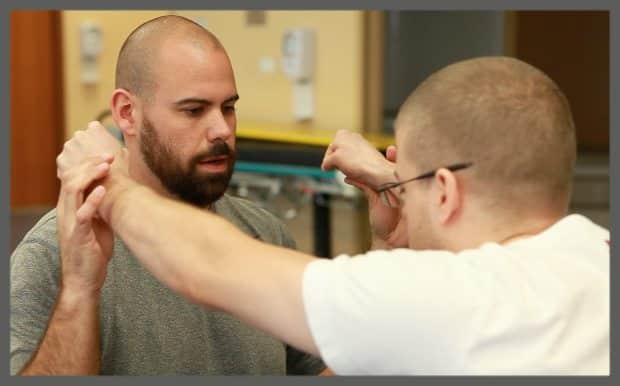
4 Ways Outpatient Physical Therapy Must Change
The average stay at a rehabilitation hospital after a spinal cord injury is 37 days.
Much of that time revolves around a grueling 3-4 hour per day routine of physical and occupational therapy that is integral to the recovery process, as messages from the brain attempt to re-communicate with the body. Unfortunately, when patients are discharged, therapy comes to a swift and premature halt. The injured move home and graduate to outpatient care. This “graduation” means therapy visits are slashed. Depending on insurance coverage, time is limited to two or three hours per week, which are then capped at a small total annually.
It’s clear to both patients and clinicians that the limited number of outpatient visits, (and the incredibly high costs of those visits) are a huge problem for the injured. Therapists spend hours each day documenting progress that begs insurance for more time.
That’s a different topic, for a different day.
What’s not as clear, and what took me three years visiting clinics around the country to understand, is that the approach of outpatient therapy at many facilities needs to change at a fundamental level.
1. Shift focus from traditional therapy to activity-based therapy
It’s time for neurologic rehab to move beyond “traditional” physical therapy that focuses on compensatory techniques (methods that show patients how to compensate for what they’ve lost by using what they have). The underlying goal of traditional therapy is to teach patients how to adapt to their injury, so they can move on with their lives as soon as possible.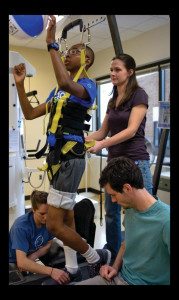
Traditional therapy certainly has its value. There is tremendous importance in learning how to adapt to injury, and find ways to gain back independence.
But, a new paradigm of neuro recovery is gaining traction at some of the elite rehab facilities around the country. It’s a shift toward activity-based therapy that focuses on strengthening the weaker muscles and nerve connections through intense functional exercise. This may include a number of different techniques: weight bearing, assisted treadmill and cycling, or aqua therapy – anything to help promote activity both below and above the injury level.
This more recent approach is based on research indicating that the nervous system has, to a certain extent, the ability to “re-train” itself through neuroplasticity. Which, simply put, is the idea that the central nervous system is not completely irrepairable. Neurons that relay information through the spinal cord try hard to repair and re-organize themselves after injury. Activity, and a blend of therapy, exercise, and repetition can help promote this.
Rehab facilities like Shepherd Center's Beyond Therapy, Craig Hospital’s PEAK Center, Magee Rehab, and others are already focusing on activity-based therapy. More facilities need to follow suit.
2. Develop wellness programs at the facility for patient off-days
Access, repetition, and more access.
That, above all else is what needs to change most about outpatient therapy.
I’ve lost count of the number of physical and occupational therapists I’ve met and worked with since my spinal cord injury. I’ve never met one who disagrees with the mantra of access and repetition. They fight a constant battle for more outpatient visits and more time to work with patients.
A combination outpatient clinic / wellness center makes too much sense not be more common.
Two physical therapy visits per week are not enough rehab for spinal cord injury. Increasing that time through exercise programs with aides and trainers on off days or after therapy visits can make up for it.
Patients should be able to come to the facility and use what they have learned from their therapists to continue their rehab. They should have access to the tools, and assistance from aides to develop a workout plan on par with their “official” outpatient visit. This access can provide the injured more rehab, AND can ensure the limited time they have with a therapist is better spent.
A therapist knows how to properly support and guide a subluxed shoulder through PNF patterns or serratus presses. A therapist can pinpoint irregular gait patterns and suggest how to fix it. A therapist’s time is best used for that. Save time on an armbike, recumbent bike, or time practicing fine motor skills for when the “official” therapy is over. Aides or personal trainers can help with that, and supervise routines the therapist may prescribe.
Neuroworx and Frazier Rehab focus on a similar style of rehab and wellness. Their model needs to be replicated.
3. Blend methods of technology and exercise
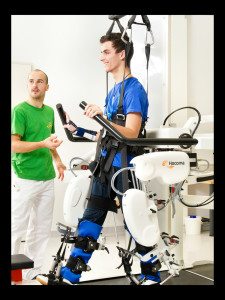 There is no singular “magic” method of physical therapy for patients with neurologic injury. Robotic therapy may be very beneficial to one person; old fashioned assisted exercise with a therapist may be the best course of treatment for another person. Neurologic recovery is far more complex than rehabbing a torn ACL or rotator cuff that has a standard protocol of care and expectation of results.
There is no singular “magic” method of physical therapy for patients with neurologic injury. Robotic therapy may be very beneficial to one person; old fashioned assisted exercise with a therapist may be the best course of treatment for another person. Neurologic recovery is far more complex than rehabbing a torn ACL or rotator cuff that has a standard protocol of care and expectation of results.
So, having access to the latest and greatest technological resources like robotics, a body-weight supported treadmill system, or electrical stimulation is fantastic, but any of these methods alone is not enough. Just like an outpatient visit simply to perform squats is not enough.
“Should we work on hip-flexors today?” isn’t going to cut it. Just like harnessing someone up in a Lokomat twice a week isn’t going to cut it.
It takes a comprehensive approach. A treatment plan that includes time spent using cutting edge equipment, and 1-on-1 exercise with experienced therapists.
For many outpatient clinics it is often one or the other.
4. Create a gym-like atmosphere, not a doctor’s office
The best and most effective physical therapy sessions are WORKOUTS. They are intense and rigorous routines that get the heart pumping and muscles stretched and fatigued. Regardless of the injury level, the wheelchair-bound must get out of their chairs and moving, not just for the sake of recovery, but for overall physical and mental health as well.
Therapists need to take a page out of a personal trainer’s playbook and combine their expertise with fitness and exercise routines.
This goes for the atmosphere in the clinic as well. The injured spend a great deal of time in doctor’s offices. Outpatient therapy should not seem like another doctor visit, sitting in a waiting room until a therapist comes to work on a few isolated muscle movements. Patients need time to loosen up on a machine like a Nu-Step, or an armbike, and get stretched by an aide before therapy begins. Muscles affected by paralysis need time to iron out spasticity and prep themselves for use. Warming up is important for an able-bodied person before a workout, and much more so for people with paralysis.
So, turn on music, open the area, and create a community. Turn physical therapy into a gym environment, not a doctor’s office.
I’ve seen this approach first-hand at Neuroworx, NextStep Fitness, Project Walk, Journey Forward, Courage Kenny, and more.
Throughout my recovery I’ve been fortunate enough to experience the practices at some of the most forward-thinking facilities in the country. Every year, when my insurance refreshes and I return to the more traditional programs in Indiana, I see the void, but I also see the potential.
Many of the resources are present. All that is missing is the catalyst for change.
For a rehab facility to truly consider itself a beacon in neurologic care, it’s not a question of if it evolves a standard of care – it’s a question of when.